Hybrid Soft-Rigid Jaw Exoskeleton
Design and modeling of a novel active hybrid rigid-soft exoskeleton for jaw motion assistance and TMD rehabilitation.
📝 UNDER REVIEW
This paper has been submitted to the 2026 IEEE International Conference on Biomedical Robotics and Biomechatronics (BioRob) and is currently under review. A preprint is available via TUprints (DOI: 10.26083/tuda-7809).
This work presents the first comprehensive computational framework for hybrid rigid-soft jaw exoskeletons, integrating a biomechanically validated $24$-muscle jaw model with deformable finite element soft-body dynamics in MuJoCo. The proposed four-tendon system combines a rigid chin cup for force transmission with a compliant facial mask for user comfort (Müller & von Stryk, 2026).

Abstract
Temporomandibular disorders (TMDs) substantially affect and impair jaw functions and thus the quality of life. Yet, powered assistance for jaw rehabilitation remains widely unexplored despite advances in exoskeletons for other extremities. To the best of our knowledge, this work presents the first comprehensive computational framework for hybrid rigid-soft jaw exoskeletons, integrating a biomechanically validated $24$-muscle jaw model with deformable finite element soft-body dynamics in MuJoCo. The proposed four-tendon system combines a rigid chin cup for force transmission with a compliant facial mask for user comfort.
Simulation-based evaluation under six configurations (TPU/Silicone materials, muscles-only/tendons-only/combined actuation) demonstrates effective trajectory tracking with mean errors of $4.60$–$6.42 \, \mathrm{mm}$ while maintaining safe interface pressures and material stresses. Critical findings reveal fundamental performance–comfort trade-offs: TPU enables efficient force transmission with lower mean strain ($11.49\%$ vs. $14.06\%$) but higher mean pressure ($12.02 \, \mathrm{kPa}$ vs. $9.89 \, \mathrm{kPa}$) than silicone. Mean tendon forces of $24.63$–$35.46 \, \mathrm{N}$ in tendons-only mode achieve effective assistance, yet combined actuation paradoxically increases biological muscle loading by $6$–$10\%$ despite improved tracking, guiding future control strategies toward biomechanical- and metabolically-aware algorithms. This validated open-source computational framework establishes essential safety constraints and design prerequisites for physical prototyping, providing a systematic path toward safe, wearable robot-assisted therapy for temporomandibular disorders.
Key Contributions:
- A novel hybrid rigid-soft jaw exoskeleton architecture balancing structural performance with user comfort and safety
- A comprehensive multi-physics simulation model enabling detailed exoskeleton–human interaction analysis
- Systematic evaluation of six configurations across two materials and three actuation modes
- A development foundation for safe, wearable robot-assisted TMD rehabilitation therapy
- Open-source release of the complete simulation framework: GitHub
Introduction
The masticatory system encompasses two temporomandibular joints (TMJs) linking the mandibular condyles to the temporal bone, with viscoelastic discs enabling six degrees of freedom (DOF) motion while absorbing substantial shear and compressive forces. This complexity renders the system prone to temporomandibular disorders (TMDs), affecting an estimated $5$–$10\%$ of the global population through musculoskeletal and neuromuscular conditions impacting the TMJs, masticatory muscles, and associated tissues. These disorders manifest through pain, restricted jaw movement, clicking sounds, muscle stiffness, and impairments in speaking, chewing, and swallowing.
Physiotherapy is the first-line treatment for TMDs, proving effective while avoiding the risks of surgical intervention. Despite significant progress in rehabilitative exoskeletons for lower and upper limbs, wearable powered assistance for jaw rehabilitation remains largely unexplored. Active jaw exoskeletons offer potential advantages over traditional manual therapy, including portability, consistent training independent of therapist availability, supervised exercise execution, progress tracking, and complex routines targeting physical and neurological rehabilitation.
Related Work
To the best of our knowledge, the literature currently reports only four active jaw exoskeletons:
- Wang et al. — A helmet-based system using dual rigid four-bar linkages coupled to a chin holder, with PID control; validated only on a passive, rigid-jaw model. An improved version later featured a central pattern generator for coordinated motion control.
- Evans et al. — A shoulder-mounted concept for vertical jaw assistance; purely conceptual, lacking simulation and prototyping.
- Kameda et al. — A semi-powered device using cables and shape-memory alloy springs; restricted to closing forces only, tested on ten healthy subjects.
- Zhang et al. — The first soft robotic approach using pneumatic actuators; validated only on a simplified physical skeleton model.
While these studies provide important insights, they all lack a systematic approach and a comprehensive simulation framework that integrates detailed biomechanics — critical for rapid prototyping, testing, and system-level evaluation of jaw exoskeletons.
System Design
Hybrid Rigid-Soft Architecture
The exoskeleton centers on a hybrid rigid-soft structure that combines a rigid chin cup for effective force transmission with a soft facial mask to ensure user comfort and safety, leveraging the inherent compliance and damping of soft materials to distribute contact forces, minimize pressure on sensitive facial tissues, and absorb high accelerations.
- Rigid chin cup — The primary interface for force transmission to the mandible. Designed to conform to the contours of the chin and lower jaw, it could be fabricated from a lightweight, rigid thermoplastic using 3D printing. The chin cup is rigidly connected to the lower jawbone, allowing effective force transmission during jaw movements.
- Compliant facial mask — A soft deformable shell based on a 3D facial skin mesh (Blender) ensuring anatomical conformity. Covers cheeks and lower jaw, distributing forces to minimize pressure points. The 2D triangular mesh ($616$ vertices, $1{,}072$ elements) is imported into MuJoCo, converted to a shell with thickness $d = 2 \, \mathrm{mm}$, and modeled using a Saint Venant-Kirchhoff hyperelastic material model via piecewise linear finite elements.
- Four-tendon actuation system — Two tendons assist jaw opening and two assist jaw closing. Both opening and closing tendons are used for lateral motions. Each cable actuator is modeled with a $75 \, \mathrm{N}$ maximum force, first-order activation dynamics ($30 \, \mathrm{ms}$ time constant), and series compliance ($10 \, \mathrm{N/mm}$ stiffness, $10 \, \mathrm{Ns/m}$ damping). These properties could represent, for instance, a combined Bowden cable, Maxon EC 45 flat motor, and $15{:}1$ gearbox system.
- Headgear frame — A rigid structure anchored to the cranium for tendon routing and actuator mounting. Four motors would be mounted on the head fixture or hips to reduce load and minimize inertia on the user’s face, with Bowden cables routing forces to the chin cup attachment points.
Biomechanical Design Requirements
The exoskeleton design is guided by biomechanical requirements derived from the literature:
| Parameter | Value |
|---|---|
| Jaw opening force (no active muscles) | $15$–$25 \, \mathrm{N}$ |
| Max voluntary opening force | $79 \, \mathrm{N}$ (men), $41 \, \mathrm{N}$ (women) |
| Max closing force (incisors) | ${\sim}100 \, \mathrm{N}$ |
| Max closing force (molars) | $> 500 \, \mathrm{N}$ |
| Vertical opening range | $35$–$60 \, \mathrm{mm}$ |
| Pure TMJ rotation range | initial $20$–$25 \, \mathrm{mm}$ |
| Lateral movement range | ${\sim}16 \, \mathrm{mm}$, up to $9.4 \, \mathrm{N}$ |
| Protrusive displacement | ${\sim}10 \, \mathrm{mm}$, up to $13.1 \, \mathrm{N}$ |
| Masseter pressure pain threshold | $119$–$163 \, \mathrm{kPa}$ |
| Perioral discomfort threshold | as low as $54 \, \mathrm{kPa}$ |
Material Configurations
Two compliant mask materials were evaluated:
| Property | TPU (eFLEX 87A) | Silicone (Sylgard 184) |
|---|---|---|
| Young’s modulus $E$ | $17.4 \, \mathrm{MPa}$ | $3.9 \, \mathrm{MPa}$ |
| Poisson’s ratio $\nu$ | $0.46$ | $0.45$ |
| Force transmission | More efficient | Less efficient |
| Comfort profile | Higher stiffness, higher contact pressure | Greater compliance, lower contact pressure |
| Ultimate tensile strength | $30.4 \, \mathrm{MPa}$ | $3.5$–$7.7 \, \mathrm{MPa}$ |
Simulation Framework
Biomechanical Jaw Model

The simulation builds on a biomechanically validated jaw model adapted from previous work (Müller & von Stryk, 2025):
- $24$ muscles with Hill-type models incorporating activation-dependent force-length-velocity relationships and passive elastic forces
- Rigid body dynamics for mandible, maxilla, hyoid, and cranium
- $5$ DOF TMJ modeled with three hinge joints (rotation) and two slide joints (coupled translation)
- $4$ ligaments for joint stabilization
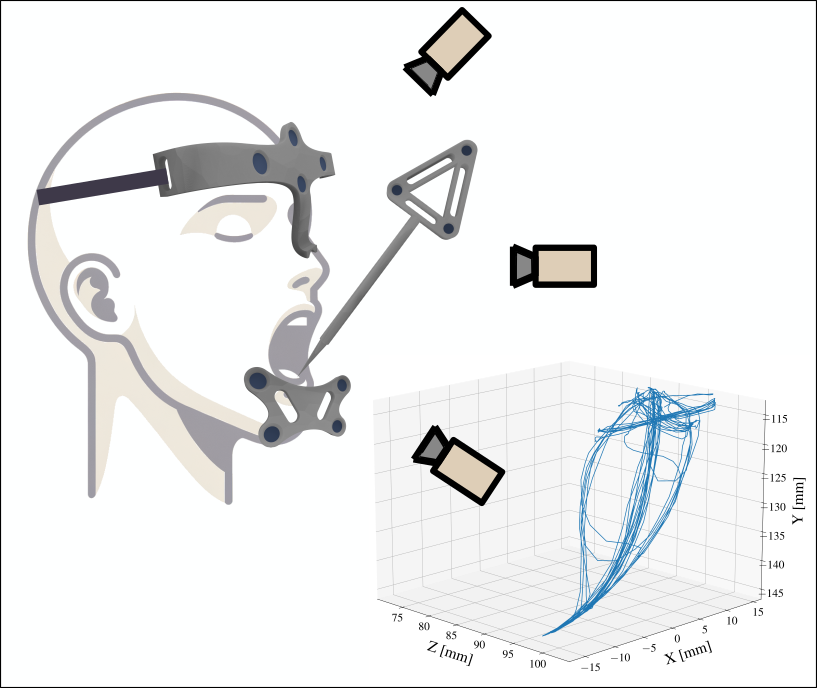
- Kinematic validation data from optical motion capture (see Jaw Tracking System) (Müller et al., 2025)
The model achieves a mean validation error of $6.63 \pm 6.84 \, \mathrm{mm}$ across all recorded motions (opening/closing, lateral movements, and chewing over $21.4 \, \mathrm{s}$). For exoskeleton experiments, the jaw opening angle is limited to $18°$ to ensure safe operation within mechanical constraints.
Deformable Soft-Body Dynamics
The model is implemented in MuJoCo 3.4.0 using hybrid rigid-soft-body dynamics capabilities with a Newton solver and implicit Euler integrator:
- Deformable FEM shells ($616$ vertices, $1{,}072$ elements, $2 \, \mathrm{mm}$ thickness) represent the soft mask
- Contact modeling between the mask and facial skin surface (rigid collision mesh, chin part attached to mandible)
- Nonlinear Saint Venant-Kirchhoff hyperelastic material model for TPU and silicone
- Coupling between rigid exoskeleton components and deformable elements
Six Evaluation Configurations
The framework was evaluated under a $2 \times 3$ factorial design:
| Muscles Only (M) | Tendons Only (T) | Combined (C) | |
|---|---|---|---|
| TPU | Biological baseline with TPU mask | Exoskeleton-driven with TPU | Muscles + tendons with TPU |
| Silicone | Biological baseline with silicone mask | Exoskeleton-driven with silicone | Muscles + tendons with silicone |
Simulation parameters:
| TPU | Silicone | |
|---|---|---|
| Time step | $1 \, \mu\mathrm{s}$ | $3 \, \mu\mathrm{s}$ |
| Real-time factor | $4.3 \times 10^{-4}$ | $1.1 \times 10^{-3}$ |
| Simulation time ($21.4 \, \mathrm{s}$ trajectory) | ${\sim}14 \, \mathrm{h}$ | ${\sim}5 \, \mathrm{h}$ |
| PID gains $(K_p, K_i, K_d)$ | $500, 70, 20$ | $200, 50, 20$ |
Simulated on Intel Core i7-6700K @ 4.0 GHz, 32 GB RAM. Data recorded at $1 \, \mathrm{kHz}$.
Control System
A basic control system was implemented to track prerecorded jaw motion trajectories. A Damped Least-Squares inverse kinematics (IK) solver computes joint configurations from desired end-effector poses, providing numerical stability near singularities through Tikhonov regularization. Given the task-space error $\mathbf{e} = \mathbf{x}_d - \mathbf{x}$ between target and current poses, joint updates are computed as:
\[\Delta \mathbf{q} = \mathbf{J}^\top (\mathbf{J}\mathbf{J}^\top + \lambda^2 \mathbf{I})^{-1} \mathbf{e}\]where $\mathbf{J}$ is the task Jacobian and $\lambda = 10^{-4}$ is the damping factor. The solver iterates until position convergence ($\lVert\mathbf{e}\rVert < 10^{-4} \, \mathrm{m}$) with step-size line search to prevent overshooting and warm-starting for trajectory continuity. MuJoCo’s forward kinematics then computes corresponding tendon-actuator lengths from joint configurations, which serve as reference inputs for PID tendon controllers.
Experimental Evaluation and Results

Trajectory Tracking Performance
Jaw trajectory tracking errors for TPU and silicone soft masks under muscles-only (M), tendons-only (T), and combined (C) actuation modes. Errors reported as mean $\mu \pm$ standard deviation $\sigma$, 95th (P95), and 99th (P99) percentiles against the recorded (Rec.) and inverse kinematics-achievable (IK-Ach.) reference trajectories:
| Rec. $\mu{\pm}\sigma$ | Rec. P95 | Rec. P99 | IK-Ach. $\mu{\pm}\sigma$ | IK-Ach. P95 | IK-Ach. P99 | ||
|---|---|---|---|---|---|---|---|
| TPU | M | $8.77{\pm}9.35$ | $32.3$ | $33.6$ | $6.42{\pm}4.47$ | $15.4$ | $17.4$ |
| T | $8.18{\pm}6.69$ | $25.0$ | $26.6$ | $6.18{\pm}3.03$ | $10.8$ | $12.9$ | |
| C | $6.94{\pm}6.81$ | $24.6$ | $26.5$ | $4.77{\pm}2.53$ | $10.4$ | $11.5$ | |
| Silicone | M | $8.59{\pm}9.06$ | $31.5$ | $32.8$ | $6.23{\pm}4.19$ | $15.0$ | $16.9$ |
| T | $7.68{\pm}6.75$ | $24.9$ | $26.6$ | $5.69{\pm}2.94$ | $10.1$ | $13.0$ | |
| C | $6.75{\pm}6.72$ | $24.4$ | $26.3$ | $4.60{\pm}2.40$ | $9.1$ | $10.7$ | |
All values in mm. M = muscles-only, T = tendons-only, C = combined.
Combined muscle-tendon actuation (C) achieves the best performance, followed by tendons-only (T) and muscles-only (M). Recorded trajectory errors systematically exceed IK-achievable errors by $2.0$–$2.4 \, \mathrm{mm}$ due to the $18°$ opening angle constraint imposed for safe operation. Against the IK-achievable reference, (C) reduces mean errors to $4.77 \pm 2.53 \, \mathrm{mm}$ (TPU) and $4.60 \pm 2.40 \, \mathrm{mm}$ (Silicone).
Silicone consistently outperforms TPU across all modes by $0.17$–$0.49 \, \mathrm{mm}$, despite requiring lower controller gains ($K_p = 200$ vs. $500$). This advantage arises from silicone’s lower stiffness ($3.9 \, \mathrm{MPa}$ vs. $17.4 \, \mathrm{MPa}$), which reduces mechanical resistance at the mask interface. P95 and P99 percentiles indicate outlier errors of $9$–$17 \, \mathrm{mm}$ during challenging segments such as high opening angles, lateral movements, and rapid transitions.
In rehabilitation applications, safety and user comfort take precedence over minimizing tracking error. Aggressive tracking generates excessive forces and pressures that can cause patient discomfort or injury, undermining therapeutic compliance.
Actuation Forces
Aggregated muscle forces (across all 24 muscles) and tendon actuator forces for all configurations. Forces reported as mean $\mu \pm$ standard deviation $\sigma$, 95th (P95), and 99th (P99) percentiles:
| Muscles $\mu{\pm}\sigma$ | Muscles P95 | Muscles P99 | Open. Tend. $\mu{\pm}\sigma$ | Open. Tend. P95 | Clos. Tend. $\mu{\pm}\sigma$ | Clos. Tend. P95 | All Tend. $\mu{\pm}\sigma$ | All Tend. P95 | ||
|---|---|---|---|---|---|---|---|---|---|---|
| TPU | M | $14.13{\pm}25.95$ | $63.0$ | $144.9$ | $0.81{\pm}0.05$ | $0.9$ | $1.17{\pm}0.02$ | $1.2$ | $0.99{\pm}0.18$ | $1.2$ |
| T | — | — | — | $26.54{\pm}26.18$ | $75.0$ | $44.37{\pm}32.25$ | $75.0$ | $35.46{\pm}30.69$ | $75.0$ | |
| C | $14.92{\pm}30.89$ | $66.4$ | $155.5$ | $43.04{\pm}29.91$ | $75.0$ | $43.33{\pm}31.71$ | $75.0$ | $43.19{\pm}30.82$ | $75.0$ | |
| Silicone | M | $9.29{\pm}19.71$ | $41.0$ | $109.6$ | $0.81{\pm}0.05$ | $0.9$ | $1.17{\pm}0.02$ | $1.2$ | $0.99{\pm}0.19$ | $1.2$ |
| T | — | — | — | $15.83{\pm}18.22$ | $50.6$ | $33.44{\pm}25.48$ | $75.0$ | $24.63{\pm}23.84$ | $75.0$ | |
| C | $10.24{\pm}25.45$ | $47.8$ | $141.5$ | $32.49{\pm}25.48$ | $75.0$ | $33.52{\pm}26.99$ | $75.0$ | $33.01{\pm}26.25$ | $75.0$ | |
All values in N. Residual tendon forces of ~1 N in (M) arise from passive series compliance.
Tendon forces in (T) and (C) approach the $75 \, \mathrm{N}$ actuator capacity at P95, with mean forces of $35.46 \pm 30.69 \, \mathrm{N}$ (TPU, T) and $43.19 \pm 30.82 \, \mathrm{N}$ (TPU, C). Silicone requires $23\%$–$31\%$ lower tendon forces than TPU, reflecting its lower stiffness — a significant efficiency advantage enabling smaller actuators or greater force margins.
Combined actuation paradox: Muscle forces increase slightly with exoskeleton assistance rather than decrease. In (C), mean muscle forces reach $14.92 \pm 30.89 \, \mathrm{N}$ (TPU) and $10.24 \pm 25.45 \, \mathrm{N}$ (Silicone), representing $6\%$ and $10\%$ elevations respectively over (M). This occurs because tendons enable reaching workspace positions that muscles alone cannot achieve, but muscles must still contribute at these configurations. Additionally, exoskeleton-enabled opening angles may stretch antagonist muscles beyond optimal length, generating passive resistance. Peak muscle forces of $66.4 \, \mathrm{N}$ (TPU) and $47.8 \, \mathrm{N}$ (Silicone) remain within safe operating limits. This highlights a critical design consideration: future control strategies should minimize muscle effort rather than just optimize tracking, including feedforward compensation for passive muscle forces and effort-aware control with EMG feedback.
Contact Force and Pressure Analysis
Contact forces and pressures at the soft mask–facial skin interface. Pressure computed from forces capped at P95 over the estimated contact area of $184.54 \, \mathrm{cm}^2$:
| Force $\mu{\pm}\sigma$ | Force P95 | Force P99 | Pressure $\mu{\pm}\sigma$ | Pressure P95 | Pressure P99 | ||
|---|---|---|---|---|---|---|---|
| TPU | M | $1.41{\pm}10.54$ | $0.7$ | $61.4$ | $8.74$ | $48.1$ | $68.0$ |
| T | $1.44{\pm}10.56$ | $1.1$ | $61.4$ | $12.02$ | $69.5$ | $105.3$ | |
| C | $1.49{\pm}10.64$ | $1.2$ | $61.7$ | $12.92$ | $77.1$ | $117.7$ | |
| Silicone | M | $1.93{\pm}13.45$ | $0.9$ | $79.7$ | $6.98$ | $58.3$ | $81.2$ |
| T | $1.91{\pm}13.28$ | $1.3$ | $79.6$ | $9.89$ | $79.0$ | $116.9$ | |
| C | $1.97{\pm}13.40$ | $1.5$ | $79.6$ | $11.09$ | $91.4$ | $133.8$ | |
Forces in N, pressures in kPa.
Silicone’s lower stiffness distributes loads more effectively, yielding lower mean pressures than TPU: $11.09 \, \mathrm{kPa}$ vs. $12.92 \, \mathrm{kPa}$ in (C). However, peak pressures (P99) show the reverse pattern: $133.8 \, \mathrm{kPa}$ (Silicone) vs. $117.7 \, \mathrm{kPa}$ (TPU). This counterintuitive result arises because silicone’s superior tracking performance reflects more aggressive controller action reaching extreme workspace positions, and the rigid facial skin collision model prevents reciprocal deformation.
Both materials remain within masseter comfort thresholds ($119$–$163 \, \mathrm{kPa}$) at P99 in (C), with TPU safely below and silicone approaching the range. Mean pressures remain well below the perioral sensitivity limit ($54 \, \mathrm{kPa}$), confirming safe operation under sustained loading. Peak pressures increase progressively across actuation modes — from (M) through (T) to (C) — revealing the fundamental performance–comfort trade-off: the $21\%$ tracking improvement from (M) to (C) requires interface pressures approaching comfort thresholds at workspace extremes.
Soft Mask Stress-Strain Analysis
Edge Stress and Strain
Concentrations at soft mask boundaries — potential failure initiation sites at material interfaces and attachment points:
| Stress $\mu{\pm}\sigma$ | Stress P95 | Stress P99 | Strain $\mu{\pm}\sigma$ | Strain P95 | Strain P99 | ||
|---|---|---|---|---|---|---|---|
| TPU | M | $0.42{\pm}0.54$ | $1.1$ | $1.4$ | $2.40{\pm}3.09$ | $6.0$ | $8.2$ |
| T | $0.42{\pm}0.58$ | $1.1$ | $1.9$ | $2.44{\pm}3.32$ | $6.5$ | $10.8$ | |
| C | $0.46{\pm}0.62$ | $1.2$ | $2.0$ | $2.63{\pm}3.57$ | $6.9$ | $11.4$ | |
| Silicone | M | $0.13{\pm}0.18$ | $0.3$ | $0.5$ | $3.41{\pm}4.52$ | $8.5$ | $12.3$ |
| T | $0.14{\pm}0.19$ | $0.4$ | $0.6$ | $3.54{\pm}4.81$ | $9.4$ | $14.5$ | |
| C | $0.15{\pm}0.20$ | $0.4$ | $0.6$ | $3.78{\pm}5.09$ | $9.9$ | $15.4$ | |
Stress in MPa, strain in %.
TPU exhibits $3.3\times$ higher edge stress but $26\%$ lower strain than silicone, directly reflecting the $4.5\times$ Young’s modulus ratio. These boundary concentrations occur during extreme jaw configurations rather than sustained loading, as confirmed by low mean values ($0.46 \pm 0.62 \, \mathrm{MPa}$ TPU, $0.15 \pm 0.20 \, \mathrm{MPa}$ Silicone).
Von Mises Equivalent Stress and Strain
Across all $1{,}072$ shell elements of the soft mask under multiaxial loading:
| Stress $\mu{\pm}\sigma$ | Stress P95 | Stress P99 | Strain $\mu{\pm}\sigma$ | Strain P95 | Strain P99 | ||
|---|---|---|---|---|---|---|---|
| TPU | M | $1.75{\pm}2.11$ | $5.3$ | $10.5$ | $10.07{\pm}12.12$ | $30.5$ | $60.1$ |
| T | $2.00{\pm}2.63$ | $6.8$ | $12.9$ | $11.49{\pm}15.11$ | $39.2$ | $73.9$ | |
| C | $1.99{\pm}2.44$ | $6.5$ | $11.6$ | $11.41{\pm}14.00$ | $37.5$ | $66.8$ | |
| Silicone | M | $0.47{\pm}0.52$ | $1.4$ | $2.7$ | $12.15{\pm}13.27$ | $34.8$ | $69.3$ |
| T | $0.55{\pm}0.62$ | $1.7$ | $3.2$ | $14.06{\pm}15.86$ | $42.8$ | $82.5$ | |
| C | $0.55{\pm}0.58$ | $1.6$ | $2.9$ | $14.17{\pm}14.82$ | $41.4$ | $75.3$ | |
Stress in MPa, strain in %.
Von Mises P99 peak stresses of $11.6 \, \mathrm{MPa}$ (TPU) and $2.9 \, \mathrm{MPa}$ (Silicone) in (C) remain well below material limits of $30.4 \, \mathrm{MPa}$ (TPU) and $3.5$–$7.7 \, \mathrm{MPa}$ (Silicone). Notably, tendons-only (T) generates slightly higher stresses than combined (C) (P95: $6.8 \, \mathrm{MPa}$ vs. $6.5 \, \mathrm{MPa}$ for TPU), because combined actuation distributes load between tendons and muscles rather than concentrating it entirely in tendon-driven transmission.
Peak strains of $66.8\%$ (TPU) and $75.3\%$ (Silicone) at P99 in (C) indicate operation near performance limits at mask boundaries during transient events, not sustained loading, as mean strains of $11.41\%$ (TPU) and $14.17\%$ (Silicone) confirm typical deformations remain moderate.
Design Trade-offs and Limitations
The evaluation reveals fundamental trade-offs:
- Stiffer materials (TPU) enable efficient force transmission but concentrate interface pressures
- Compliant materials (silicone) distribute loads at the cost of greater deformation
- Combined actuation improves tracking but paradoxically increases biological muscle loading
Key limitations include the underactuated four-tendon design restricting independent 3D motion control, and modeling simplifications: rigid facial skin collision, omitted tendon-mask routing dynamics, and idealized rigid chin cup–mandible attachment. Additionally, opening tendon forces require stable reaction points not yet addressed in the current head fixture design. The restricted $18°$ workspace, single-subject validation, and computational expense further constrain immediate applicability. Aesthetics and long-term wearability remain unquantified.
Conclusion and Outlook
This work addresses an important gap in powered jaw rehabilitation research by presenting a validated computational framework that integrates biomechanical musculoskeletal dynamics with deformable finite-element modeling. The hybrid rigid-soft architecture demonstrates effective tendon-driven assistance while revealing fundamental performance–comfort trade-offs: TPU and silicone both maintain safe operation, with inherent trade-offs between force transmission efficiency and pressure distribution. This simulation-based evaluation establishes essential safety constraints and design principles that must be validated computationally before physical prototype development, as direct hardware experimentation on sensitive facial structures and the temporomandibular system poses unacceptable risks without prior virtual testing.
Future Directions
Model fidelity improvements:
- Deformable facial skin representations with patient-specific geometries
- TMJ disc models for intra-articular load analysis
- Expanded tendon routing with contact dynamics
- Realistic mandible attachment interfaces (dental braces, intraoral appliances)
- Multi-layer architectures combining structural TPU with compliant silicone inner layers
- Gradient stiffness designs to address stress concentrations
Control sophistication:
- Model predictive control with reinforcement learning-optimized parameters
- EMG-driven intent detection for intuitive human-robot collaboration
- Effort-aware algorithms that minimize metabolic cost to address the paradoxical increase in muscle loading
- Feedforward compensation for passive muscle forces
Expanding functional capabilities:
- Protrusive motion support and additional actuation DOF
- Alternative actuation technologies (shape memory alloys, pneumatic artificial muscles, optimized electric drives)
- Body-anchored head fixtures via shoulder straps for stable opening tendon reaction points
- Wearable sensing integration for real-time biomechanical feedback and personalized rehabilitation protocols
Technical Specifications
| Parameter | Value |
|---|---|
| Simulation engine | MuJoCo 3.4.0 (hybrid rigid-soft-body dynamics) |
| Solver / Integrator | Newton solver, implicit Euler integrator |
| Jaw model | $24$ muscles (Hill-type), $5$ DOF TMJ, $4$ ligaments |
| Actuation | $4$ tendons, $75 \, \mathrm{N}$ max force, $30 \, \mathrm{ms}$ activation |
| Series compliance | $10 \, \mathrm{N/mm}$ stiffness, $10 \, \mathrm{Ns/m}$ damping |
| Soft mask mesh | $616$ vertices, $1{,}072$ elements, $2 \, \mathrm{mm}$ shell |
| Material model | Nonlinear Saint Venant-Kirchhoff hyperelastic |
| Materials | TPU ($E = 17.4 \, \mathrm{MPa}$, $\nu = 0.46$), Silicone ($E = 3.9 \, \mathrm{MPa}$, $\nu = 0.45$) |
| Contact area | ~$184.54 \, \mathrm{cm}^2$ |
| Validation trajectory | $21.4 \, \mathrm{s}$ (opening/closing, lateral, chewing) |
| Data rate | $1 \, \mathrm{kHz}$ |
| Language | Python |
Licensing and Availability
The complete simulation framework is released as open source to facilitate further research and development.
GitHub: https://github.com/paulotto/hybrid-jaw-exo-sim
Authors
- Paul-Otto Müller — Simulation, Systems Optimization and Robotics Group, Technical University of Darmstadt
- Oskar von Stryk — Simulation, Systems Optimization and Robotics Group, Technical University of Darmstadt
This work was partially supported by the German Research Foundation DFG within RTG 2761 LokoAssist (Grant no. 450821862).
Citation
@InProceedings{Mueller2026b,
author = {Müller, Paul-Otto and von Stryk, Oskar},
booktitle = {2026 IEEE International Conference on Biomedical Robotics
and Biomechatronics (BioRob), Edmonton, Canada},
title = {Design and Modeling of a Novel Active Hybrid Exoskeleton
for Jaw Motion Assistance},
year = {2026},
month = aug,
publisher = {TUprints, Darmstadt},
doi = {10.26083/tuda-7809}
}